You're probably here because you or someone you love has been affected by psoriasis. Let's start by acknowledging that psoriasis is indeed a tricky thing, often showing up uninvited and trying to steal the limelight. However, knowledge is power, and understanding this pesky condition can help us conquer it together!
Psoriasis, for those still figuring it out, is an autoimmune skin condition. The body's immune system, which usually defends us from infections and diseases, mistakenly attacks healthy skin cells, leading to the signature red, scaly patches. And believe it or not, around 125 million people around the globe are sharing this journey with you.
But don't worry! This article will serve as your personal guide to understanding, managing, and thriving despite psoriasis.
Understanding Psoriasis
What is Psoriasis?
Let's jump right in and get to know this unwelcome visitor named psoriasis. It's actually an autoimmune skin condition, meaning our body's defense system gets a bit confused and starts seeing normal skin cells as the enemy.
This results in an accelerated skin cell growth cycle - instead of a month, it takes only days for new skin cells to rise to the skin's surface.
This fast-paced cell turnover doesn't give the old skin cells enough time to shed, leading to the buildup that causes those red, scaly patches we know as psoriasis.
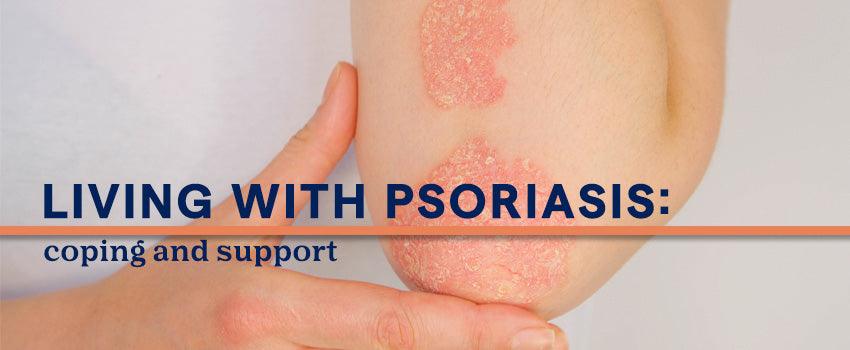
Common symptoms include red patches of skin covered with thick, silvery scales, dry, cracked skin that may bleed, itching, burning, or soreness.
Types of Psoriasis
Now, let's get a bit more specific. Psoriasis is not a one-size-fits-all condition - it comes in several different forms, each with its own set of characteristics.
The most common type is Plaque Psoriasis. It comes with dry, raised, red skin patches covered in silvery scales. These patches can appear anywhere on your body, but they're typically found on the scalp, elbows, knees, and lower back.
Then there's Guttate Psoriasis, which often starts in children or young adults. It's marked by small, water-drop-shaped, scaling lesions on the trunk, arms, or legs.
Pustular Psoriasis, which is less common, appears as clearly defined, raised bumps filled with white, noninfectious pus.
Remember, each type can vary in severity and will respond differently to treatments, so it's crucial to consult with your dermatologist for a proper diagnosis.
Psoriasis and Associated Health Risks
Beyond the skin, psoriasis carries with it a few more potential risks. One significant concern is Psoriatic Arthritis, which affects up to 30% of people with psoriasis. It causes painful, swollen joints and can lead to permanent damage if not treated promptly.
Also, having psoriasis can increase your likelihood of developing certain other conditions, like cardiovascular diseases. Research suggests that the inflammation driving psoriasis may also influence the development of heart diseases.
Psoriasis doesn't just affect physical health. It can have a considerable impact on mental health, leading to feelings of self-consciousness, embarrassment, and even depression. The social and emotional effects can be just as significant as the physical ones.
While these potential risks might seem daunting, remember, being aware of them is the first step towards effective management. Your healthcare team can guide you through managing these risks, so you're not alone on this journey.
Coping with Psoriasis
Medical Management
Managing psoriasis often begins with seeking medical help. Several effective therapies are currently available to soothe symptoms and keep flare-ups at bay. Topical treatments, such as creams and ointments, can be particularly helpful for mild to moderate psoriasis. They work by reducing inflammation and slowing down excessive skin cell production.
For more stubborn or widespread psoriasis, light therapy or systemic medications might be prescribed. These treatments work throughout the body to suppress the overactive immune response.
Recently, there has been a growing interest in biologic drugs. These are medications derived from living organisms that target specific parts of the immune system. They can be quite effective but are generally reserved for moderate to severe cases of psoriasis.
It's essential to remember that treatment plans are individualized - what works for one person may not work for another. So, consistent communication with your dermatologist is crucial.
Lifestyle Adjustments
Taking care of your overall health can greatly aid in managing psoriasis. Eating a balanced diet, rich in fruits, vegetables, lean proteins, and whole grains, can support your immune system and promote healthier skin. It's also a good idea to limit foods that trigger inflammation, such as processed foods, refined sugars, and unhealthy fats.
Physical activity is another cornerstone of psoriasis management. Regular exercise can help reduce inflammation, boost your mood, and maintain a healthy weight. Remember, research has shown that people with psoriasis who are overweight or obese tend to have more severe symptoms.
Don't forget the importance of quality sleep. Adequate rest can help the body recover and reduce inflammation, leading to fewer psoriasis flare-ups. If you're having trouble sleeping, speak with your doctor for advice or consider relaxation techniques such as meditation or deep breathing exercises.
Skin Care Routine
Proper skin care is essential when living with psoriasis. Daily moisturizing can help prevent dryness, reduce itching, and maintain the skin's natural barrier. Look for creams and ointments that are fragrance-free and include ingredients like hyaluronic acid or ceramides, which help to hydrate and repair the skin. Some over-the-counter products containing coal tar or salicylic acid may also help to reduce scaling.
When bathing, avoid hot water as it can strip the skin of natural oils. Instead, use warm water and keep your showers short. Choose mild, fragrance-free soaps to prevent irritation. After bathing, gently pat your skin dry with a towel and apply moisturizer immediately to lock in the moisture.
Remember, skincare is a personal journey, and what works for one person may not work for another. Always consult with your dermatologist before starting a new skin care product or routine.
Support for People Living with Psoriasis
Mental Health and Psoriasis
Dealing with psoriasis goes beyond the skin. It's a condition that also chips away at our mental and emotional well-being. It's common for individuals living with psoriasis to experience feelings of embarrassment, frustration, and even social isolation. This emotional toll can drive up stress levels, triggering even more psoriasis flare-ups - a stressful loop, to say the least.
Managing this emotional turbulence is an essential part of effective psoriasis care. Mental health professionals can provide valuable techniques to cope with stress, elevate self-esteem, and enhance emotional health.
Additionally, incorporating practices like mindfulness-based stress reduction can prove beneficial. In fact, a study has shown its positive effects on individuals with chronic skin conditions, including psoriasis.
Psoriasis Support Networks
As you navigate through your journey with psoriasis, you don't have to go it alone. Having supportive loved ones can make a big difference, providing emotional support and practical help when you need it.
Sometimes, though, you may feel the need to connect with people who are in the same boat. That's where psoriasis support groups come in. These can be in-person groups or online communities, offering a platform to share experiences, exchange tips, and give and receive encouragement. Resources like the National Psoriasis Foundation offer a wealth of support, including online forums and communities.
Educating Others About Psoriasis
Fighting the stigma and misinformation surrounding psoriasis begins with education. Initiate conversations with your friends, family, colleagues, or even your child's school. Letting them understand what psoriasis is - and what it isn't (hint: it's not contagious!) - can foster empathy and understanding.
Your journey with psoriasis, your experiences and your knowledge, can serve as a beacon for others going through similar situations. Remember, knowledge empowers us all and it's our greatest weapon in fighting psoriasis-related stigma.
Conclusion
In essence, psoriasis doesn't define you or your loved ones. It's a complex condition that touches physical and mental health, but with the right resources and approach, it's entirely manageable. Remember, you're not alone in this journey - there's a world of support available, from medical professionals to online communities.
Take control of your health and well-being today, not just to cope, but to thrive. Psoriasis may be part of your story, but it doesn't write it. You do.
So, let your narrative shine with strength, resilience, and hope. After all, you're not just living with psoriasis – you're living a life of empowerment.



Leave a comment
This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.